Door-to-Door Delivery: Why Reliability Matters More Than Speed
Door-to-door delivery is often described as a convenience. For healthcare organizations, it’s something far more critical. It’s a way to reduce uncertainty in systems where uncertainty is expensive.
When a delivery is late, undocumented, or unclear, the cost isn’t just the delivery fee. It’s staff time spent reconstructing what happened, patients waiting longer than they should, compliance questions that take hours to resolve, and clinical teams pulled away from care. In healthcare logistics, even small breakdowns in coordination can ripple into real operational risk — and many organizations don’t realize it until it’s too late. The early signs your medical courier is lacking often appear long before a delivery is officially marked “failed.”
Industry research on the hidden costs of healthcare logistics shows that inefficiencies across the supply chain quietly drive higher labor costs, delayed care, and mounting administrative burden, especially when accountability breaks down between handoffs.
Door-to-door delivery exists to prevent that. It assigns a single, accountable partner from pickup through final handoff, with clear ownership over timing, documentation, and escalation. When something matters, responsibility doesn’t fragment.
This guide explains what door-to-door delivery actually means, how it compares to other healthcare delivery models, when it’s worth the cost, and how healthcare leaders evaluate providers when reliability, compliance, and visibility are non-negotiable.
What Door-to-Door Delivery Actually Means
Door-to-door delivery is a logistics model where a single provider manages pickup, transport, tracking, delivery confirmation, and documentation from start to finish, with full accountability for timing, compliance, and proof of delivery.
That ownership is the point.
In many delivery setups, responsibility fragments along the way. One company picks up. Another transports. A third handles the last mile. When something goes wrong, teams spend more time figuring out who was responsible than fixing the problem itself.
With door-to-door delivery, that ambiguity disappears.
A single provider is accountable not just for moving an item, but for tracking it in real time, confirming delivery, documenting chain of custody, and escalating issues before they become failures. Timing, documentation, and compliance all sit with one owner.This model is becoming increasingly important as healthcare delivery grows more distributed. As care shifts beyond hospital walls—to clinics, labs, pharmacies, and patient homes—delivery networks must support direct-to-patient logistics, a segment projected to exceed $21 billion by 2025. In that environment, handoffs multiply quickly. Clear ownership is what keeps them from turning into risk.
Why the Difference Between Delivery Models Matters
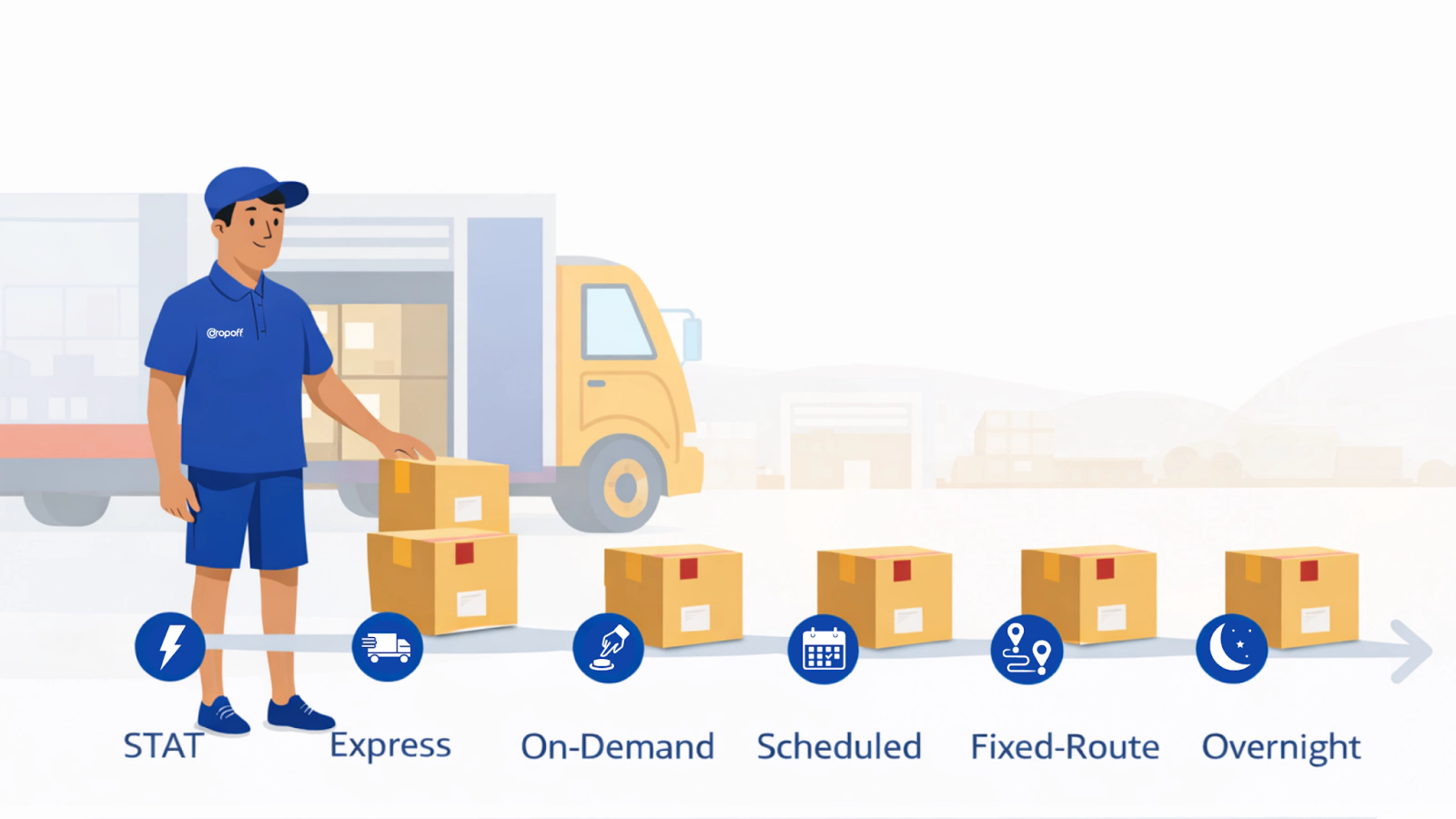
Terms like courier service, last-mile delivery, and door-to-door delivery are often used interchangeably. Operationally, they are not the same—and confusing them is where problems start.
Courier services optimize for speed.
National carriers optimize for scale.
Door-to-door delivery optimizes for accountability when failure has consequences.
That distinction shapes how these models behave in real healthcare environments.
Last-mile delivery focuses on the final leg only. Courier services typically operate job by job, with limited standardization or visibility beyond pickup and drop-off. National carriers move massive volumes efficiently, but they are optimized for scale, not adaptation. When conditions change, flexibility is limited.
Door-to-door delivery is built for situations where failure has consequences. It prioritizes ownership over handoffs and accountability over throughput. That difference is why healthcare organizations rely on it when timing, documentation, and compliance cannot be optional.
Healthcare supply chains today are more distributed than ever. Care now flows across clinics, labs, pharmacies, and patient homes, often with multiple stakeholders involved in a single delivery path. In that environment, logistics systems must support not just movement of goods, but visibility, compliance, and resilience across decentralized networks.
In healthcare logistics, the real challenge isn’t getting something from point A to point B. It’s being able to answer what happened, when it happened, and who was responsible—so care teams can stay focused on outcomes instead of exceptions.
How Door-to-Door Delivery Works in the Real World

On paper, the process looks straightforward.
Pickup. Transport. Delivery.
In real operations, reliability is decided by what happens between those steps.
A well-run door-to-door delivery begins with verified pickup and continues with active monitoring throughout transit. Delivery windows are defined, not implied. Handoffs are confirmed, not assumed. In healthcare settings, this also means documented chain of custody and clear escalation protocols when something deviates from plan.
Those details aren’t administrative overhead. They’re what allow clinical and operations teams to trust the delivery without having to chase it.
This is where many delivery models quietly break down. GPS can tell you where a vehicle is, but it can’t tell you whether a specimen was handed to the right person, whether access issues delayed a delivery, or whether a missed handoff is about to cascade into a larger problem later in the day. By the time those questions surface, the damage is often already done.
True visibility means understanding not just where a shipment is, but what has happened to it at every step — and whether someone is accountable for acting when conditions change.
As Sean Spector explains:
“If you map every failure we’ve ever had, they fall into two buckets: something broke that shouldn’t have, or someone didn’t know it broke. That second one is worse. Visibility isn’t about GPS. It’s about accountability — who knew, who acted, how fast. That’s the chain that actually keeps healthcare running.”Fast delivery only matters if it’s also confirmed, documented, and defensible. In healthcare, uncertainty is often more disruptive than delay — because teams can adjust to known problems, but they can’t plan around silence.
When Door-to-Door Delivery Makes Sense
Door-to-door delivery is rarely chosen because it’s the cheapest option. It’s chosen when the cost of failure outweighs the cost of delivery.
That calculation shows up most clearly in healthcare workflows where timing, documentation, and accountability directly affect patient care and operational continuity.
Consider specimen transport between clinics and labs. A delayed or undocumented handoff doesn’t just mean a late delivery—it can mean recollection, patient rescheduling, and delayed diagnosis. Pharmacy deliveries carry similar risk. When medications arrive late or without confirmation, teams scramble to reroute doses, trigger STAT replacements, or field compliance questions that consume far more time than the delivery itself.
The stakes are just as high with surgical kits and medical devices. A missing or late kit can idle an operating room, push procedures off schedule, and cascade into staffing and resource conflicts that ripple across the day. STAT runs between facilities are often the clearest example: these are moments where speed matters, but certainty matters more. Teams need to know exactly where something is, when it will arrive, and who is accountable if conditions change.
In all of these scenarios, success isn’t defined by how fast something moves. It’s defined by how confidently teams can rely on the delivery without checking on it.
When internal teams find themselves chasing couriers, reconstructing timelines, or answering “what happened?” after the fact, door-to-door delivery often lowers total operational cost—even if the per-run rate is higher. The savings come from fewer disruptions, less rework, and fewer hours spent managing exceptions instead of care.
When Door-to-Door Delivery Isn’t the Right Tool
Not every shipment needs this level of control.
Door-to-door delivery is designed for situations where timing, documentation, and accountability materially affect outcomes. When those factors aren’t present, the added oversight can introduce unnecessary cost and friction.
Low-urgency shipments, bulk freight, and non-sensitive parcels are often better served by simpler delivery models that prioritize efficiency over precision. Using door-to-door delivery in these cases doesn’t add value—it just adds process.
Knowing when not to use door-to-door delivery is part of using it well. Providers who are clear about those boundaries tend to be more reliable partners, because they’re optimizing for fit, not forcing every shipment into the same solution.
Generic Medical Couriers vs. Specialized Last-Mile Partners
Many companies offer medical delivery. Far fewer are built around how healthcare actually operates.
Generic medical couriers often treat healthcare as one job type among many, a common outcome of the difference between carriers and couriers and how their operating models are designed. They move packages efficiently, but the systems behind those movements are rarely designed for clinical workflows. Tracking may stop at basic GPS pings. Proof of delivery can be minimal. Escalation tends to happen after a failure, once someone notices something went wrong.
Specialized last-mile partners operate differently because the assumptions are different.
At Dropoff, healthcare deliveries are designed around compliance, chain of custody, and operational visibility from the start. Couriers are trained to work in clinical environments, not just to complete a route. Deliveries follow documented handoffs, with tracking that captures meaningful events, not just location. Proof of delivery is recorded in a way that supports audits, internal review, and real accountability when questions arise.
Details that seem small in other industries matter here. Uniformed drivers reduce friction at handoff. Clear identification builds trust with staff who are already under pressure. Consistent processes mean fewer interruptions and fewer follow-ups after the delivery is complete.
As Sean Spector puts it:
“Visibility isn’t about GPS. It’s about accountability. Who knew. Who acted. How fast.”
That distinction is why healthcare organizations lean toward specialized partners when the cost of uncertainty is higher than the cost of delivery.
What Cost-Sensitive Healthcare Leaders Actually Optimize For
Healthcare leaders aren’t optimizing for the lowest delivery rate. They’re optimizing to avoid downstream disruption.
In healthcare operations, delivery failures rarely stay isolated. A single undocumented specimen delivery can turn a five-minute run into hours of follow-up across lab staff, clinicians, and compliance teams.
A missed or undocumented specimen delivery doesn’t just cost a courier fee. It triggers recollection, staff rework, patient rescheduling, and delayed diagnosis.
A pharmacy delivery that arrives late or without confirmation often leads to STAT re-runs, after-hours staffing, and compliance follow-up that far exceed the original delivery cost.
The same dynamic plays out in procedural settings. When a surgical kit or medical device arrives late, the impact isn’t confined to logistics. Procedures are delayed. Operating rooms sit idle. Teams are rescheduled. What looked like a small delivery decision quickly becomes a scheduling and cost problem that ripples across the day.
Seen through that lens, the economics shift. In each case, the delivery cost itself is marginal compared to the cost of failure—and experienced leaders know it.
As Nick Araiza puts it:
“Cheaper couriers look good on paper, until the first failure wipes out every dollar you saved.”
That’s the ROI calculation healthcare leaders are actually making: not what the delivery costs, but what it prevents.
How to Evaluate a Door-to-Door Delivery Partner
When reliability matters, the difference between providers shows up quickly—usually in how they answer a small set of operational questions.
Start with proof of delivery. Not whether it exists, but how it’s captured, shared, and stored. In healthcare settings, confirmation isn’t just a timestamp. It’s evidence that stands up to internal review and external scrutiny.
Then look at exception handling. What happens when a delivery can’t be completed as planned? Is escalation proactive and real-time, or does the customer only find out after something has already failed?
Training matters just as much as technology. Couriers working in healthcare environments need to understand HIPAA expectations, clinical workflows, and how to operate in spaces where mistakes have consequences. (For reference, this HIPAA compliance guide for medical couriers outlines the baseline expectations most providers should meet.)
Measurement is another tell. Can performance be tracked consistently over time, or only explained anecdotally? Reliable partners can show trends, not just individual successes.
Finally, ask who owns the problem when something goes wrong. Clear answers signal clear accountability. Vague answers usually mean the risk shifts downstream to your team. Many organizations only recognize the warning signs your medical courier is lacking after delivery issues start showing up in their operations.
Why Healthcare Organizations Choose Dropoff
Healthcare organizations choose Dropoff when delivery becomes part of patient care, not just logistics.
Dropoff specializes in high-stakes, time-critical deliveries where accountability and documentation matter as much as speed. That focus shapes its healthcare logistics operations, with clear ownership from pickup through final handoff and processes built to surface issues early rather than explain them later.
Instead of relying on anecdotes or after-the-fact reporting, Dropoff measures what healthcare teams actually need to know: on-time performance, first-attempt delivery success, and proof-of-delivery confirmation that stands up to internal review. When questions arise, teams aren’t left reconstructing timelines or guessing what happened.
The result is fewer interruptions, fewer escalations, and more confidence that critical deliveries are being handled the way healthcare operations require.

Often, yes—on a per-delivery basis. But healthcare organizations don’t evaluate door-to-door delivery in isolation.
The relevant comparison isn’t the delivery rate. It’s the total cost of failure. Missed or undocumented deliveries can trigger recollection, rescheduling, after-hours staffing, compliance follow-up, and internal rework that quickly exceeds the original delivery cost. Door-to-door delivery reduces those downstream expenses by minimizing uncertainty and eliminating handoff gaps.
For high-stakes deliveries, the model is often less expensive operationally, even if it costs more upfront.
That depends on the provider’s operating model.
Professional door-to-door providers escalate in real time. Instead of silently marking a delivery as failed, they notify stakeholders, confirm next steps, and document what occurred. This allows healthcare teams to make informed decisions quickly—rerouting, rescheduling, or authorizing alternatives before the situation becomes disruptive.
Silence is usually the most expensive outcome.
Door-to-door delivery can support HIPAA compliance, but compliance isn’t automatic.
HIPAA depends on how sensitive materials are handled, documented, and secured throughout transit. That includes courier training, chain-of-custody documentation, proof of delivery, and audit-ready records. The delivery model matters less than the process discipline behind it.
Healthcare organizations should evaluate whether a provider’s practices align with HIPAA expectations—not just whether they claim compliance.
In healthcare, proof of delivery goes beyond a timestamp.
A robust door-to-door delivery includes time-stamped confirmation, recipient verification, and digital records that document who received the item, when the handoff occurred, and whether any exceptions were noted. These records should be accessible for internal review and external audits.
The goal isn’t just confirmation—it’s defensibility when questions arise later.
Door-to-door delivery is most valuable when timing, documentation, and accountability materially affect outcomes.
That includes specimen transport, pharmacy delivery, surgical kits, medical devices, and STAT runs between facilities. In these scenarios, teams don’t just need speed. They need certainty—and a clear owner when something changes.